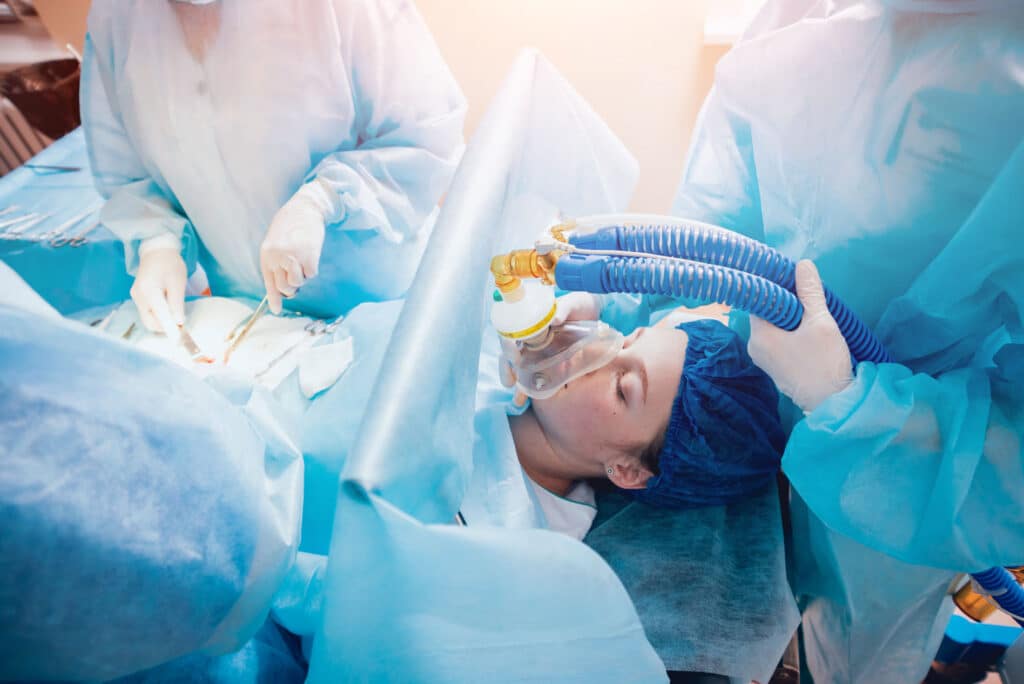
One crucial aspect that ensures the safety and success of spine surgeries is anesthesia. Anesthesia plays a vital role in minimizing pain, providing comfort, and ensuring patient immobility during the procedure.
Understanding the basics of anesthesia for spine surgery is essential for patients and their families to make informed decisions and alleviate any concerns. Here we give you a general scope of the role of anesthesia in your spine surgery in Laguna Beach, CA!
First…What Is Spine Surgery?
Spine surgery is a complex surgical procedure that is performed to alleviate various conditions and disorders of the spinal column, spinal cord, and spinal nerves, such as degenerative disc disease, compression fractures, spinal instability, and spinal curves.
Although spine surgery can also significantly improve the overall quality of life, the patient’s healing process will likely require several weeks of physical therapy and rest.
Different age groups have their own specific reasons for needing spine surgery. Among younger patients, the most common problems treated are degenerative spine disease and herniated disks, and when it comes to elderly patients over 60 years old, they most commonly undergo spine surgery for spinal stenosis.
Whatever the reason for spine surgery, anesthesia is essential in any.
What Are the Most Common Types of Spinal Surgeries?
- Spinal fusion: This involves joining two or more vertebrae together to stabilize the spine, often using bone grafts, metal rods, screws, or plates. This type of procedure has recently been refined into Transforaminal lumbar interbody fusion, or TLIF, helping lower the risk of muscle damage.
- Discectomy: It is a procedure to remove all or part of a damaged or herniated disc that is causing nerve compression, resulting in pain, weakness, or numbness.
- Laminectomy: This is the removal of the lamina, a part of the vertebra that covers the spinal canal, to relieve pressure on the spinal cord and nerves, usually due to spinal stenosis.
- Microdiscectomy: A minimally invasive procedure similar to discectomy, where only a small portion of the herniated disc is removed through a small incision, reducing tissue damage and recovery time.
- Foraminotomy: It is a surgery to widen the opening (foramen) through which the spinal nerves exit the spinal canal, relieving pressure caused by conditions like bone spurs or herniated discs.
- Artificial disc replacement: A surgical alternative to fusion, where a damaged disc is replaced with an artificial disc, maintaining motion and flexibility in the spine. This includes lumbar disc replacement and cervical disc replacement.
- Vertebroplasty and kyphoplasty: Procedures used to treat vertebral compression fractures. In vertebroplasty, bone cement is injected into the fractured vertebra, while in kyphoplasty, a balloon is first inserted to create space before injecting the cement.
- Spinal decompression: This procedure helps alleviate pressure on the spinal cord or nerves by removing bone or tissue causing the compression, commonly used for conditions like spinal tumors or cysts.
- Scoliosis surgery: For severe cases of scoliosis (abnormal sideways curvature of the spine), surgery may involve spinal fusion, corrective rods, or implants to straighten and stabilize the spine. In the case of spinal curves, there are two different kinds that need surgical correction. The first condition, often known as idiopathic scoliosis, manifests as an aberrant spine curve for unexplained causes. The second kind of curvature is typically linked to other conditions that harm bones, muscles, and nerves.
- Spinal cord stimulator implantation: This surgery involves the placement of a device that delivers electrical impulses to the spinal cord, helping to alleviate chronic pain by interfering with pain signals.
How is Anesthesia Used During Spine Surgery?
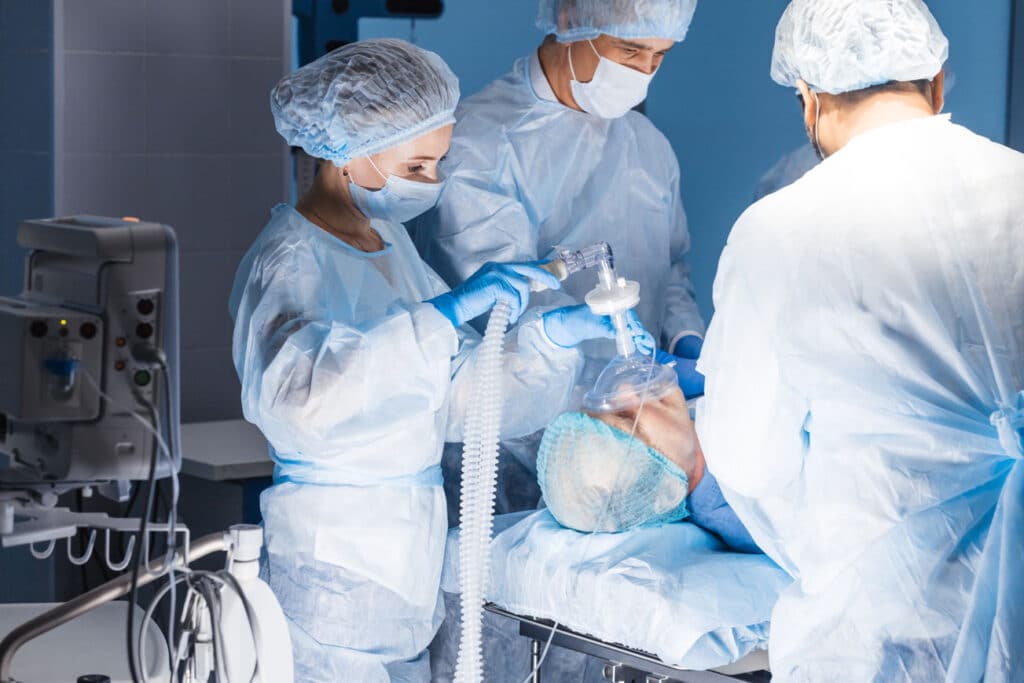
General anesthesia is the form of anesthesia that is typically chosen for all types of surgical procedures involving the spine because it improves patient tolerance, provides a secure airway, allows for better surgical exposure while using muscle relaxants, allows for an early postoperative exam without the confounding effects of traditional epidural anesthetics, and provides better surgical control. For example, general anesthesia is used to perform surgical correction of spinal curvature (scoliosis) or any type of cervical spine surgery.
Spine surgery might also use epidural and spinal anesthesia. Epidural anesthesia involves injecting a local anesthetic and sometimes a tiny quantity of opioids into the epidural space, the outermost region of the spinal canal. This treatment numbs surgical nerves to relieve pain, enabling patients to stay awake or be lightly sedated.
However, spinal anesthesia includes injecting the anesthetic directly into the cerebrospinal fluid in the subarachnoid space, numbing a broader area below the injection. This causes total anesthesia and muscle relaxation, necessitating extensive sedation during surgery. The choice between epidural and spinal anesthesia depends on the procedure, patient preference, and doctor’s advice.
Both epidural and spinal anesthesia, though, are less common in this procedure. They are used mostly for lumbar spine surgery or interventions in general that do not require a breathing tube on the patient, like with all cervical spine surgery. Or, in cases of awake spine surgery, which is where the patient is nominally awake but can’t feel anything below their neck. Awake spine surgery is rare and recommended only in special circumstances.
Next, we give you the process that anesthesia goes through during your spinal surgery:
Before Spine Surgery
On the day of surgery, you will meet with your anesthesiologist. Depending on the type of surgery, you might need to consult an anesthesiologist before the scheduled operation if you have a complex medical condition.
You’ll be questioned about your health history, current medications, allergies, past anesthesia experiences, and general well-being.
Your heart, lungs, and airway will all be closely inspected as well. The anesthetic strategy will then be discussed with you by your anesthesiologist. A member of the pain management team will meet with you to go over a plan for making sure you are comfortable after surgery.In order to help you unwind before surgery, we may occasionally administer medicine to you orally or intravenously (IV). Additionally, this drug induces amnesia, so you might not remember the anxiety you felt in the run-up to the operation.
During Spine Surgery
In order to begin spinal surgery, anesthesia, either IV medicine or, for younger patients, gas through an anesthetic mask, is administered. Based on your needs, your anesthesiologist will select the ideal type of anesthesia. Most, if not all, spinal surgeries are carried out while the patient is in the prone position, which is essentially lying face down on the operating table. The prone position is the posture that is utilized to gain access to the back of the head, neck, and spine during spinal surgery. Some rare back surgeries are carried out in the supine position (facing up.)
After you fall asleep while in the prone position, the nurses and doctors will take further measures to protect your security and welfare. A breathing tube may also be inserted, along with more intravenous (IV) lines.
Additionally, other drugs might be employed to prevent interfering with any spinal cord and nerve function monitoring that might take place during your operation. Neurophysiologic monitoring is the name given to this particular monitoring. The surgical team will use a number of monitors to assess your vital signs and the electrical activity of the heart, blood oxygen levels, and respiration.
In order to do neurophysiologic monitoring, the patient must be asleep when specific monitoring electrodes are placed on them. The neurophysiologist continuously tracks a number of nervous system processes as you sleep so that any possible issues can be identified right away.
When neurophysiologic monitoring is used, the anesthesiologist will collaborate with the neurophysiologist and surgeon to administer anesthesia that keeps you safe and comfortable but does not significantly interfere with monitoring.
Blood Transfusion
Blood transfusions are frequently necessary during spine surgery. This is especially true if the patient suffers from a nerve or muscle condition that has caused a spinal curvature.
This kind of self-directed blood transfer won’t be achievable at other times. Your anesthesiologist will carefully watch you decide if a blood transfusion is necessary.
Your health and well-being come first, even though the surgical team makes every effort to use as little blood transfusion in the operating room as possible.
Arterial Line
Additionally, when you fall asleep, a unique blood pressure monitor (an arterial line) is implanted because it’s crucial that the surgeons carefully monitor blood pressure during your spine surgery.
Similar to a standard IV, an arterial line is inserted into an artery rather than a vein (often in the wrist). This enables us to carefully monitor your blood pressure and collect blood samples for testing in the lab.
The period following the procedure will see the arterial line remaining in place.
After Surgery
After surgery, some people are awakened immediately in the operating room when the surgery is finished. Others must be kept asleep after surgery, usually no more than one to two days.
Under these circumstances, you will remain deeply asleep with a breathing tube in place and will require a ventilator.
If you are awake and meet the criteria, you will be transferred to the post-anesthesia recovery room (PACU) and eventually to your assigned room.
A member of the anesthesia team will visit the day after surgery to make sure that you are pleased with the anesthesia care you received while in our operating room. You will also immediately be asked if you’re feeling any postoperative pain, whether it’s too much, out of the ordinary, or common.
Medications Use
The drugs administered after surgery are made to encourage sound sleep, offer effective pain relief, and relax the muscles.
Some of the medications used to treat someone who just had spine surgery include pain medications such as opioids, nonsteroidal anti-inflammatory drugs (NSAIDs), and muscle relaxants. Opioids are often prescribed in the immediate post-operative period to manage severe chronic pain. NSAIDs help reduce inflammation and relieve pain. Muscle relaxants are used to alleviate muscle spasms that may occur as a result of the surgical intervention. Additionally, patients may be prescribed antibiotics to prevent infection and blood thinners to prevent blood clots. The specific medications prescribed will depend on the individual’s condition, the procedure’s extent, and medical history. It is important for patients to follow their healthcare provider’s instructions and take medications as directed to optimize their recovery.
Wake-Up Test
As part of the monitoring of nerve function, a “wake-up” test may be performed. In this test, the anesthetic is lightened to see if the patient is able to move his or her feet in response to a verbal command. This test typically takes less than five minutes.
The anesthetic is then deepened until a patient wakes up after the procedure is completed. The wake-up test is not uncomfortable and is usually not remembered after surgery.
Risks and complications
Anesthesia for spine surgery, like any medical procedure, carries certain risks and potential complications. It is important for patients and their families to be aware of these risks in order to make informed decisions and alleviate any concerns. Some potential risks and complications of anesthesia for spine surgery include:
- Adverse effects and reactions to anesthesia drugs: Some individuals may have allergic reactions or adverse reactions to the drugs used for anesthesia. These reactions can range from mild to severe and may include symptoms such as nausea, vomiting, difficulty breathing, or changes in blood pressure. This is why vital signs monitoring is so important from the start and why there are alternatives like awake spine surgery for patients who can’t tolerate or don’t want general anesthesia. In the case of awake spine surgery, epidural anesthesia might also be an option, especially for interventions on the lumbar spine.
- Respiratory complications: Anesthesia can affect the respiratory system, leading to complications such as lung infections, pneumonia, or difficulty breathing. Patients may require assistance with breathing through the use of a ventilator during and after surgery.
- Cardiovascular complications: Anesthesia can have an impact on the cardiovascular system, potentially causing changes in heart rate, blood pressure, or rhythm. This can increase the risk of heart attack, stroke, or other cardiovascular complications.
- Nerve damage: Although extremely rare, nerve damage can occur as a result of anesthesia administration. Nerve damage can lead to temporary or permanent loss of sensation, weakness, or paralysis.
- Postoperative pain and discomfort: Patients may experience postoperative pain and discomfort immediately or hours after surgery. Anesthesia manages and alleviates this pain, but individual responses can vary. The nursing staff will be especially crucial when treating pain after spine surgery, as they’ll be the ones in constant communication with the patient.
- Blood transfusions: Spine surgery may sometimes require blood transfusions, especially in cases where there is significant blood loss. While efforts are made to minimize blood loss and the need for transfusions, they carry their own set of risks, such as transfusion reactions or infections.
- Infection: Any surgical procedure carries a risk of infection. This can include infections at the surgical site and systemic infections that can affect other parts of the body.
It is important to note that the risks and complications associated with anesthesia for spine surgery can vary depending on factors such as the patient’s overall health, the complexity of the surgery, and the specific anesthesia techniques used. The anesthesiologist will assess each patient individually and take measures to minimize these risks while ensuring the safest possible outcome.
Book Your Appointment with Dr. Hamid Mir!

Doctor Hamid R. Mir is a board-certified orthopedic spine surgeon near Laguna Beach, CA with fellowship training in combined neuro and orthopedic spine surgery techniques who’s based in Orange County, CA. He has 18 years of experience in minimally invasive spine surgeries using advanced microscopic techniques.
With his expertise, compassionate approach, and medical team, you can trust Dr. Mir to guide you through the diagnosis, treatment, and recovery process, ensuring the best possible outcomes for your spinal health. Don’t wait; schedule your appointment today and take the first step towards a healthier spine.
FAQ
How are pre-existing medical conditions handled during surgery?
The surgical team carefully and strategically handles pre-existing medical conditions during spine surgery. The patient’s medical history and pre-existing conditions are thoroughly evaluated before the surgery. This helps the surgical team to anticipate and address any potential complications that may arise during or after the procedure.
The surgical team may work in collaboration with the patient’s primary care physician or specialist to optimize their overall health condition before the procedure. This may involve adjusting medications, managing chronic conditions, and implementing lifestyle changes.
How is my condition monitored during surgery?
During the surgery itself, the surgical team takes extra precautions to minimize risks associated with pre-existing conditions. This may include closely monitoring vital signs, using specialized equipment, and adjusting surgical techniques as necessary. This involves continuously measuring and tracking the patient’s heart rate, blood pressure, oxygen saturation levels, and temperature. These vital signs are important indicators of a patient’s overall condition and can help the surgical team identify any changes requiring immediate attention.
Additionally, the surgical team may employ specialized monitoring techniques during spine surgery. For example, intraoperative neurophysiological monitoring (IONM) is often used to assess the integrity of the patient’s nervous system during the procedure. This involves monitoring the electrical activity of the brain, spinal cord, and peripheral nerves to ensure they function properly. By continuously monitoring these signals, the surgical team can identify any potential spinal nerve damage or complications and take appropriate action to minimize risks to the patient.
How do they administer anesthesia for back surgery?
Anesthesia for back surgery is typically administered through a combination of general anesthesia and regional anesthesia techniques. General anesthesia involves the use of medications to induce a state of unconsciousness, ensuring that the patient does not feel any pain or discomfort during the surgery. It is usually administered intravenously, allowing the anesthesiologist to continuously monitor and adjust the patient’s level of sedation. General anesthesia also involves the use of a breathing tube to maintain proper oxygenation and ventilation throughout the procedure.
In addition to general anesthesia, regional anesthesia techniques such as epidural or spinal anesthesia may be used for back surgery. These techniques involve the injection of local anesthetic medication near the spinal cord to numb the nerves in a specific region of the back. Epidural anesthesia is commonly used for procedures involving the lumbar spine (lower back,) while spinal anesthesia is often preferred for surgeries involving the lower spine and lower extremities. These regional anesthesia techniques provide additional pain relief during and after the surgery, reducing the need for high doses of general anesthesia and minimizing postoperative pain.



