ALIF surgery is performed utilizing general anesthesia. A breathing tube (endotracheal tube) is placed and the patient breathes with the assistance of a ventilator during the surgery. Preoperative intravenous antibiotics are given. Patients are positioned in the supine (lying on the back) position, generally using a special, radiolucent operating table. The surgical region (abdominal area) is cleansed with a special cleaning solution. Sterile drapes are placed, and the surgical team (a spine surgeon and vascular surgeon) wears sterile surgical attire such as gowns and gloves to maintain a bacteria-free environment.
A 3-8 centimeter (depending on the number of spinal levels to be fused) transverse or oblique incision is made just to the left of the belly button. The abdominal muscles are gently spread apart but are not cut. The peritoneal sac (containing the intestines) is moved to the side, as are the major large blood vessels. Special retractors are used to allow the surgeon to visualize the anterior (front part) aspect of the intervertebral discs. After the retractor is in place, an X-ray confirms that the appropriate spinal level(s) is identified.
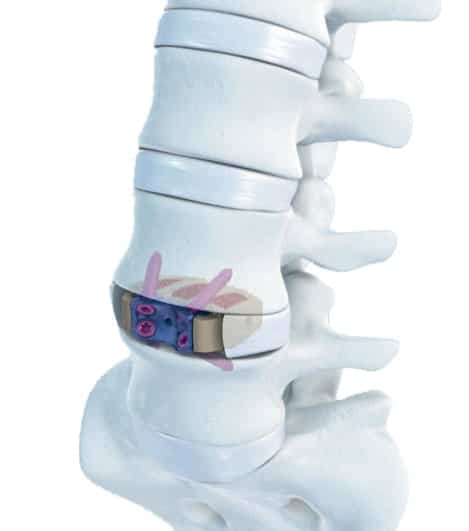
The intervertebral disc is then removed using special biting and grasping instruments. Special distractor instruments are used to restore the normal height of the disc, as well as to determine the appropriate size spacer to be placed. A bone spacer (metal or plastic spacers may also be used) is then carefully placed in the disc space. Typically, this spacer or cage contains bone graft material. In some circumstances, a metal plate and screws are used to reinforce the graft. Fluoroscopic X-rays are taken to confirm that the spacer is in the correct position.
The wound area is usually washed out with sterile water containing antibiotics. The deep fascial layer and subcutaneous layers are closed with a few strong sutures. The skin can usually be closed using special surgical glue, leaving a minimal scar and requiring no bandage.
The total surgery time is approximately 2 to 3 hours, depending on the number of spinal levels involved.
Although the risks of spinal surgery are minimal, it is important to be aware of them. Some potential common spine surgery complications include:
- Bleeding
- Risk of infection
- Blood clots (deep vein thrombosis)
- Dural tear
- Nerve damage
You should also contact your surgeon, as well as your doctor if you’ve experienced any of the following after being released from the hospital:
- Fever
- Leg pain, weakness, or numbness that gets worse
- Painful or swollen calf muscles
- Issues with your balance or walking
- Increased back pain
- Fluid leaking from the wound
- Issues with managing your bladder or bowels or passing urine
- Swelling, redness, a rise in temperature, or suspicion that the wound is infected.
In order to avoid any problems, be sure to dutifully follow the surgeon’s instructions regarding home care for 2 weeks after surgery.